Herpes Zoster — commonly known as shingles — is a painful skin condition caused by the reactivation of the varicella-zoster virus (VZV), the same virus responsible for chickenpox. After a person recovers from chickenpox, typically during childhood, the virus does not completely leave the body. Instead, it remains dormant in the sensory nerve roots near the spinal cord and brain. Years or even decades later, the virus can reactivate, traveling along nerve pathways to the skin and causing a distinctive, often blistering rash. This reactivation is more likely to occur when the immune system becomes weaker due to aging, stress, chronic illness, or immunosuppressive treatments.
For many adults — especially those aged 50 and older or individuals with weakened immune systems — shingles is more than just a temporary skin eruption. The condition is often accompanied by severe nerve pain, burning sensations, tingling, or heightened skin sensitivity that can persist even after the rash has healed. One of the most common and debilitating complications is postherpetic neuralgia (PHN), a chronic nerve pain that may last for months or even years. In some cases, shingles can also affect the eyes (herpes zoster ophthalmicus), potentially leading to vision problems, or cause neurological complications. Fortunately, vaccination provides strong protection by boosting immunity against VZV reactivation, significantly reducing the risk of shingles and its long-term complications.
Understanding Herpes Zoster (Shingles)
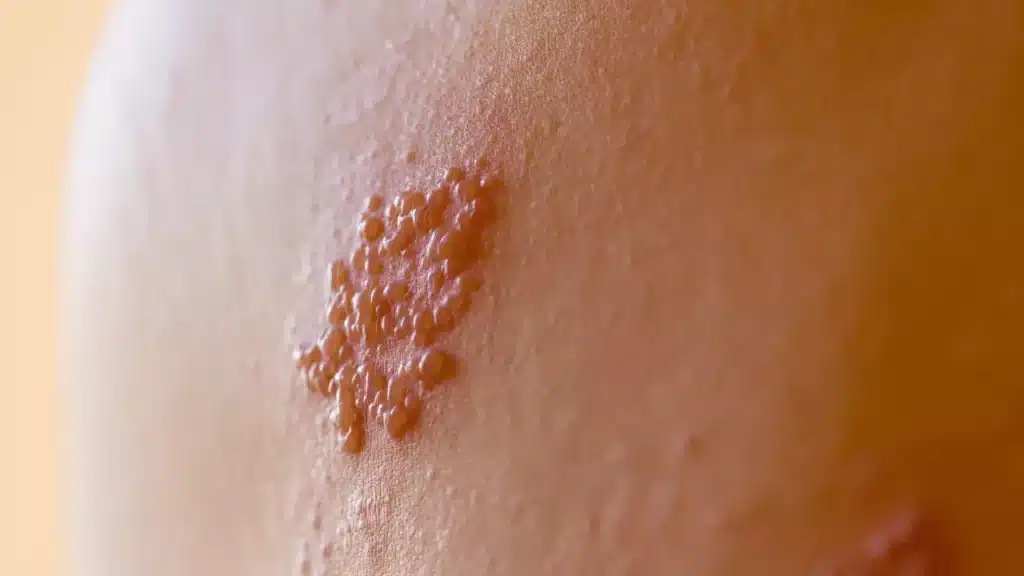
Herpes Zoster — or shingles — results from the reactivation of the varicella-zoster virus in the body. After a primary infection with chickenpox (varicella), the virus lies dormant in the nervous system for years or even decades. When the immune system weakens due to age, stress, or illness, the virus may reactivate and cause shingles.
Shingles typically manifests as a painful, blistering skin rash localized to one side of the body. It often follows a single dermatome — a strip of skin supplied by one nerve. The pain can be intense and is sometimes followed by complications that can significantly impact quality of life.
Common Complications of Shingles
- Post-herpetic neuralgia (PHN): Long-lasting nerve pain that persists long after the rash heals.
- Herpes zoster ophthalmicus: Shingles involving the eyes, which can threaten vision.
- Skin infections: Secondary bacterial infections of the rash.
- Neurological complications: Rare but serious conditions like encephalitis.
The risk of these complications increases significantly in older adults and those with weakened immune systems.
Why Vaccination Matters
Vaccination is one of the most effective and reliable strategies to prevent shingles and its potentially serious complications. While the chickenpox vaccine is routinely administered during childhood to prevent primary varicella infection, the shingles vaccine is specifically designed for adults whose immunity to the varicella-zoster virus (VZV) has naturally declined over time. Health authorities primarily recommend shingles vaccination for individuals aged 50 years and older, as immune function gradually weakens with age, a process known as immunosenescence. In addition, certain younger adults may also benefit from vaccination, particularly those with chronic medical conditions, autoimmune diseases, cancer, HIV infection, or those undergoing treatments such as chemotherapy or long-term corticosteroid therapy that suppress the immune system.
Without vaccination, shingles is remarkably common and affects approximately one in three people during their lifetime, with the incidence rising significantly after the age of 60. The condition not only causes a painful rash but also increases the risk of complications such as postherpetic neuralgia (PHN), a persistent nerve pain that can severely impact quality of life. Importantly, experiencing shingles once does not provide guaranteed lifelong immunity, and recurrence can occur, especially in individuals with weakened immune defenses. Vaccination helps strengthen the body’s immune response against VZV reactivation and reduces both the likelihood of developing shingles and the severity of symptoms if it does occur.
Meet Shingrix: The Modern Herpes Zoster Vaccine

Shingrix (recombinant zoster vaccine, RZV) is currently the most advanced and effective vaccine approved for the prevention of herpes zoster and post-herpetic neuralgia. It is a non-live, recombinant vaccine that stimulates the immune system to build strong defense against the virus.
How Shingrix Works
Shingrix contains a purified protein (glycoprotein E) from the varicella-zoster virus combined with an adjuvant system that boosts immune response. It does not contain live virus, so it cannot cause shingles. The adjuvant enhances both cellular and humoral immunity, which is essential for strong and lasting protection.
Efficacy and Effectiveness
Clinical trials have consistently shown that Shingrix offers high levels of protection, with more than 90 % efficacy in preventing herpes zoster in adults aged 50 or older. Protection remains strong even in those aged 70 and older.
Research also suggests that Shingrix:
- Reduces the risk of post-herpetic neuralgia (chronic nerve pain)
- Maintains effectiveness for many years after vaccination
- Performs significantly better than older shingles vaccines like Zostavax, which had lower and decreasing effectiveness over time
Schedule of Vaccination
Shingrix is administered as a two-dose series:
- First dose (Day 0)
- Second dose typically 2 to 6 months later
Completing both doses is essential to achieve optimal immunity and long-term protection.
Who Should Get the Shingles Vaccine?
Health authorities recommend Shingrix for all adults aged 50 years and above, even if they recall having had shingles or chickenpox in the past. Age is a major risk factor for reactivation of VZV and the development of shingles.
Younger Adults at High Risk
Shingrix is also recommended for adults 18 years and older who are at increased risk due to:
- Weakened immune systems
- Certain chronic illnesses
- Treatments like chemotherapy, radiation, or long-term steroid therapy
These individuals have a higher likelihood of severe shingles and complications.
Benefits Beyond Shingles Prevention
While the primary purpose of shingles vaccination is to prevent herpes zoster and its complications, emerging research suggests that its benefits may extend beyond protecting the skin and nerves. Scientists are increasingly exploring how preventing viral reactivation can positively influence overall systemic health. Because shingles is associated with inflammation that can affect multiple organ systems, reducing the likelihood of viral reactivation may also help lower the risk of inflammation-related conditions. Although these findings are still being studied, they open promising perspectives about the broader protective effects of vaccination.
Better Heart Health
Some observational studies have suggested a possible link between shingles vaccination and a reduced risk of cardiovascular events such as stroke and heart attack. Herpes zoster infection is known to trigger inflammatory responses and vascular changes that may temporarily increase the risk of blood clot formation. In fact, the risk of stroke has been observed to rise shortly after a shingles episode, particularly in older adults. By preventing shingles or reducing its severity, vaccination may help minimize these inflammatory and vascular effects, thereby potentially lowering short- and long-term cardiovascular risks. While the exact biological mechanisms are still under investigation, reduced systemic inflammation is believed to play a key role.
Potential Brain Health Benefits
Emerging evidence also indicates a possible association between shingles vaccination and improved cognitive health outcomes in older adults. Some large-scale population studies have reported a lower incidence or delayed onset of dementia among individuals who received the shingles vaccine compared to those who did not. One hypothesis is that preventing viral reactivation reduces chronic neuroinflammation, which has been linked to cognitive decline. Another possibility is that vaccination enhances immune system regulation in ways that indirectly support brain health. Although these findings are promising, they remain under active research, and further long-term clinical studies are needed to establish a clear cause-and-effect relationship.
While more research is required to confirm and better understand these associations, the potential systemic benefits strengthen the overall value of shingles vaccination. In addition to protecting against painful rashes and long-term nerve damage, vaccination may contribute to broader protective effects that support cardiovascular and cognitive health in aging populations.
Safety and Side Effects

Like any medical intervention, Shingrix vaccination can cause side effects — most of which are temporary and mild to moderate.
Common Reactions
After receiving Shingrix, you may experience:
- Pain, redness, or swelling at the injection site
- Muscle pain
- Fatigue and tiredness
- Headache
- Fever or chills
- Gastrointestinal discomfort
These side effects typically subside within a few days.
Rare but Serious Events
Severe allergic reactions are possible but extremely uncommon. Signs include swelling of the face or throat, difficulty breathing, or rapid heartbeat — in these cases, immediate medical attention is needed.
A rare condition called Guillain-Barré syndrome has been observed in isolated cases after vaccination, but its connection to the vaccine is still being studied.
Who Should Not Receive Shingrix?
Shingrix is generally not recommended for:
- Individuals with known severe allergic reactions to vaccine components
- Pregnant or breastfeeding women, unless advised otherwise by a physician
- People actively experiencing shingles or chickenpox
As always, consult with a qualified health professional before vaccination.
Where to Get the Herpes Zoster Vaccine
Getting vaccinated with Shingrix is simple and accessible in many clinics and health-care facilities around the world — including in Bali.
Saline Bali Clinic — Trusted Provider for Shingles Vaccination
For residents and visitors in Bali, Saline Bali Clinic offers the Herpes Zoster Vaccine using Shingrix, one of the most effective recombinant vaccines available today. According to their service information, Shingrix at Saline Bali Clinic is administered under professional medical supervision, ensuring safety, comfort, and optimal immune protection.
Saline Bali Clinic is known for its high quality of care, patient-centered approach, and comprehensive health services, making it a trusted choice for vaccinations and preventive care in Bali.
For more detailed information about the Herpes Zoster Vaccine at Saline Bali Clinic, you can visit their dedicated vaccine page or chat here.
Why You Should Consider the Herpes Zoster Vaccine
Herpes zoster, while often underestimated can cause severe pain, long-term neuralgia, and serious complications, particularly in older adults and those with weakened immune systems. Vaccination with Shingrix represents a powerful prevention tool that has transformed shingles protection, offering over 90 % effectiveness and long-lasting immunity.
By completing the recommended two-dose series, individuals can significantly reduce their risk of developing shingles and its complications, improving overall health outcomes. The vaccine’s safety profile is well-established, and most side effects are temporary and manageable.
Whether you are turning 50, have chronic health concerns, or simply want to stay ahead of age-related disease risks, the Herpes Zoster Vaccine is a valuable investment in long-term health. For those in Bali seeking a professional and trusted vaccination service, Saline Bali Clinic is an excellent choice for receiving the Shingrix vaccine under expert care.
Frequently Asked Questions (FAQ) About Herpes Zoster
What is Herpes Zoster?
Herpes Zoster, also known as shingles, is a viral infection caused by the reactivation of the varicella-zoster virus (VZV), the same virus that causes chickenpox. After a person recovers from chickenpox, the virus remains dormant in nerve tissue and can reactivate later in life, leading to a painful rash and nerve-related symptoms.
What are the early symptoms of shingles?
Early symptoms often include tingling, burning, itching, or sharp pain on one side of the body or face. These sensations are usually followed by the appearance of a red rash that develops into fluid-filled blisters. Some people may also experience fever, headache, fatigue, or sensitivity to light.
Who is at higher risk of developing shingles?
Shingles is more common in adults aged 50 years and older, as immunity naturally declines with age. Individuals with weakened immune systems due to medical conditions such as cancer, HIV, autoimmune disorders, or those undergoing chemotherapy or long-term steroid treatment are also at increased risk.
Can shingles occur more than once?
Yes, shingles can recur. Although many people experience it only once, having shingles does not guarantee lifelong immunity. Recurrence is possible, especially in older adults or those with compromised immune systems. Vaccination can significantly reduce the risk of future episodes.
How can shingles be prevented?
The most effective way to prevent shingles and its complications is through vaccination. The shingles vaccine is recommended primarily for adults aged 50 and older, and for certain younger individuals at higher risk. Vaccination reduces the likelihood of developing shingles and lowers the risk of complications such as postherpetic neuralgia, a chronic nerve pain condition.



